A nerve plexus is a plexus of intersecting nerves. A nerve plexus is composed of afferent and efferent fibers that arise from the merging of the anterior rami of spinal nerves and blood vessels. There are five spinal nerve plexuses, except in the thoracic region, as well as other forms of autonomic plexuses, many of which are a part of the enteric nervous system. The nerves that arise from the plexuses have both sensory and motor functions. These functions include muscle contraction, the maintenance of body coordination and control, and the reaction to sensations such as heat, cold, pain, and pressure. There are several plexuses in the body, including:Spinal plexuses
Cervical plexus - serves the head, neck and shoulders
Brachial plexus - serves the chest, shoulders, arms and hands
Lumbosacral plexus
Lumbar plexus - serves the back, abdomen, groin, thighs, knees, and calves
Subsartorial plexus - below the sartorius muscle of thigh
Sacral plexus - serves the pelvis, buttocks, genitals, thighs, calves, and feet
Pudendal plexus
Coccygeal plexus - serves a small region over the coccyx
Autonomic plexuses
Celiac plexus - serves internal organs
Auerbach's plexus - serves the gastrointestinal tract
Meissner's plexus - serves the gastrointestinal tract
Pharyngeal plexus of vagus nerve - serves the palate and pharynx
Cardiac plexus - serves the heart
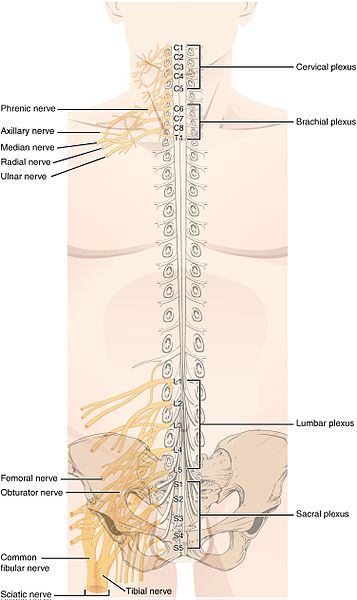
Superimposed image of the spinal plexuses on a human back.
In human anatomy, the sacral plexus is a nerve plexus which provides motor and sensory nerves for the posterior thigh, most of the lower leg and foot, and part of the pelvis. It is part of the lumbosacral plexus and emerges from the lumbar vertebrae and sacral vertebrae (L4-S4). A sacral plexopathy is a disorder affecting the nerves of the sacral plexus, usually caused by trauma, nerve compression, vascular disease, or infection. Symptoms may include pain, loss of motor control, and sensory deficits.
Sacral plexus


